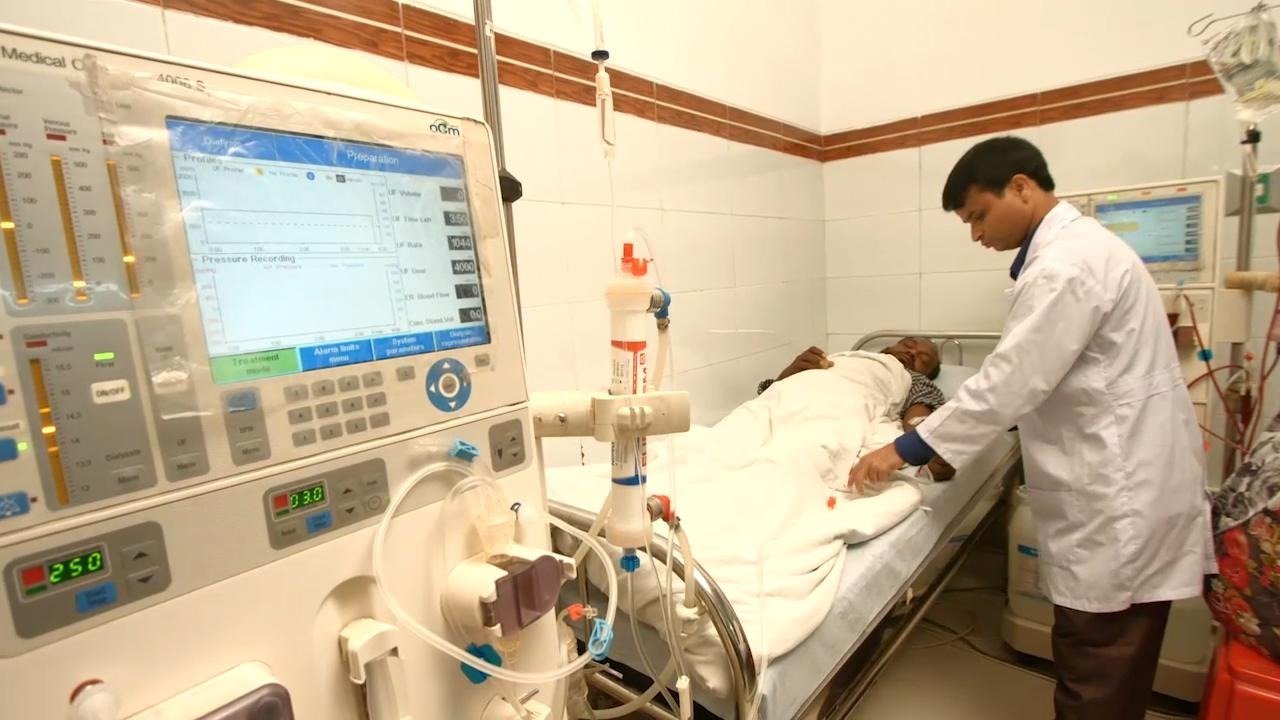
Managing anemia is a critical part of care for patients with chronic kidney disease (CKD), especially those undergoing dialysis. For years, erythropoiesis-stimulating agents (ESAs) have played an important role in helping raise hemoglobin levels and reduce the need for blood transfusions. However, new research is raising an important clinical question: could higher-dose ESA use be linked to an increased cancer risk in dialysis patients?
As healthcare continues to move toward more personalized and risk-aware treatment strategies, this topic is becoming increasingly relevant for nephrologists, dialysis providers, and patients alike.
Why ESAs Matter in Dialysis Care
Anemia is a common complication in patients with advanced kidney disease because damaged kidneys produce less erythropoietin, the hormone responsible for stimulating red blood cell production. ESAs were developed to address this problem and have become a widely used part of anemia management in nephrology care.
For many patients, ESAs can improve quality of life by helping reduce fatigue, weakness, and symptoms related to low hemoglobin. But like many effective therapies, their use must be balanced against potential risks.
The Concern: Could Higher ESA Exposure Carry Long-Term Risks?
Recent reporting on emerging research suggests that high-dose ESA use may be associated with a greater risk of cancer compared with lower-dose use in dialysis patients. While this does not necessarily prove direct causation, it does raise an important concern about whether treatment intensity could influence long-term outcomes in vulnerable patient populations.
This is especially significant because dialysis patients often already carry a high burden of chronic illness, inflammation, immune dysfunction, and complex medication exposure. In such populations, even modest shifts in risk can be clinically meaningful.
Why This Finding Matters Clinically
The question is not whether ESAs should suddenly be abandoned. Rather, the conversation is shifting toward how they should be used more carefully and strategically.
This emerging discussion highlights several important clinical priorities:
1. Dose Matters
Not all ESA use may carry the same level of concern. If higher doses are linked to worse long-term outcomes, clinicians may need to place even greater emphasis on using the lowest effective dose needed to manage anemia safely.
2. Individualized Treatment Is Essential
Dialysis patients are not a uniform group. Age, cancer history, inflammatory burden, nutritional status, iron deficiency, and comorbid disease all influence how anemia should be managed. A one-size-fits-all approach is no longer enough.
3. Risk-Benefit Decisions Must Stay Patient-Centered
For some patients, the benefits of anemia correction may still clearly outweigh potential risks. For others, a more conservative strategy may be appropriate. The key is thoughtful, individualized decision-making.
A Broader Shift in Anemia Management
This discussion also reflects a larger trend in nephrology: moving away from simply “correcting lab values” and toward outcome-focused care.
In the past, aggressive anemia correction was sometimes viewed as a straightforward goal. Today, clinicians are increasingly focused on the bigger picture:
- Symptom improvement
- Cardiovascular safety
- Hospitalization risk
- Transfusion avoidance
- Long-term complications
That shift is important because in complex chronic diseases like kidney failure, treatment success is not defined by numbers alone. It is defined by how safely and effectively patients can be supported over time.
What Patients Should Understand
For patients on dialysis, headlines like these can understandably create anxiety. But it is important to remember that treatment decisions should never be based on isolated headlines alone.
Patients should speak with their nephrologist or care team if they have questions about:
- Why they are receiving ESA therapy
- What dose they are on
- Whether alternative or supportive strategies are available
- How their anemia is being monitored over time
Open communication matters. When patients understand the purpose, risks, and monitoring behind a treatment plan, they are better equipped to participate in their care.
The Importance of Ongoing Research
The relationship between anemia treatment, ESA dosing, and cancer risk is complex, and more research will likely be needed to fully understand it. Still, this emerging evidence is valuable because it encourages a more careful and evidence-based approach to treatment.
In modern medicine, progress does not always come from replacing therapies. Often, it comes from learning when, how, and for whom they should be used most responsibly.
Conclusion
ESAs remain an important part of anemia management in dialysis care. But new concerns around high-dose ESA exposure and possible cancer risk highlight the need for continued vigilance, clinical judgment, and individualized care planning.
As the evidence evolves, the focus should remain clear: using the right treatment at the right dose for the right patient always with safety and long-term outcomes at the center of care.